Home » Health
Category Archives: Health
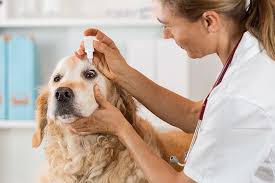
Why Choose A Holistic Veterinarian
How To Choose The Right Veterinarian For Your Pet
It can be difficult to know what to look for when looking for a Veterinarian for your pet. You may have moved and left behind a vet with whom you have great rapport or you may have a new pet and are overwhelmed by all those big ads in the yellow pages. While there is no magic formula to guarantee a positive experience and high-quality care for your pet, there are a few ways to simply evaluate the hospital and veterinarian you choose.
Ask friends for recommendations
Before making an appointment you should check with friends and neighbors who own pets. Find out who they use and why. It is a good idea to get several different opinions since no one person will be liked by everyone. You want to get a sampling of opinions.
A visit to the clinic
Next, visit the clinic before making the appointment. The staff should be happy to answer any questions about the practice. It is also legitimate to request a tour at a time that is mutually convenient. There may be times of the day when a tour is not advisable but your request should be granted at some point.
The staff
Evaluate the front office staff? Are they helpful? Friendly? Do they acknowledge you when you walk in or are you ignored? What is the overall appearance of the clinic? Is it clean? Odor free? What is the attitude of the staff toward the other clients who may be present? How about to those on the other end of the phone line? You can learn a lot by just observing.
Your first appointment
If you make the appointment you will have a chance to meet with the doctor and the assistants. (Of course, you may have already met some of these people if you stopped in the office). You should evaluate these people in the same manner as previously described. Are the assistants helpful and friendly? Are they kind to your pet? Are they rough in handling the animal or gentle?
Meeting the veterinarian
How about the doctor? Does he/she take time to listen to your concerns? Are you given enough time to explain and ask questions? How is his/her rapport with your pet? Does he/she talk to your animal and try to establish a relationship before starting the exam? Is your pet called by name? Does the doctor take time to do an exam and address your concerns? Do you feel comfortable asking questions? Are you questions answered?
If your pet is ill or if some type of in-hospital procedure is required is everything well explained?
Make sure you communicate your needs to the doctor
It is always appropriate to ask specific questions about procedures, medications, anesthetics etc. It is also a good idea to tell the doctor exactly what you expect. If you treat your pet as a family member and want the doctor to feel free to do whatever he/she feels is necessary you should say so. If finances are a major concern that should be mentioned at the outset so there will be no surprises.
Verify location
The right veterinarian for you, aside from being a qualified and recommended pet doctor, should work at a clinic that you can get to easily. Especially if you have a pet emergency, you don’t want to have to go far once you make an appointment.
How close you want your vet to be can depend on the health of your pet. If you have a younger, healthy animal, proximity can get a little lax. If you have an older pet and you have concerns, try to find a vet a little closer.
If you’re worried about access to pet care, once you select your regular vet, ask them about the closest emergency animal hospital. Emergency vets, which are typically open 24-hours, are available in certain locations when it’s impossible to see your regular veterinarian. If something goes wrong with your pet and you can’t wait for your clinic to open, this is where you should go. Some conditions that may lead to an emergency visit for your pet include:
- Difficulty breathing
- Repeated vomiting and/or diarrhea
- Excessive bloating
- An accident with trauma
- Ingesting a foreign object
- Not eating, drinking or urinating

Choosing a Vet for Your Cat? Consider These Factors
It’s not just for shots; you’ll need a cat veterinarian for a number of reasons. Maybe you’re a new cat parent, your family just moved, or your cat is in need of medical care. Whatever the reason, it’s important to find a cat vet with whom you—and your feline friend—are comfortable seeing on a regular basis.
What’s the best way to go about finding a vet that’s right for you and your cat? Here are your options.
Friends and Reviews
Consider asking close friends who have cats about their choice. Another good way to find a vet, of course, is to explore reviews of local facilities online. But take reviews of a cat hospital with a grain of salt, according to Dr. Patty Khuly, as they often reflect subjective cases of financial coverage, rather than the care they provide.
What’s Important toYou
Once you have a list of potential vets to choose from, there are several factors to consider that can help you whittle it down. What’s most relevant to you? Price, location, hours, wait times, and bedside manner should all come to mind. Does the vet offer grooming and boarding? If your cat suffers from a disease or recurrent health problem, a vet that specializes in this issue might be the best route. Ultimately, consider the factors that are important to you specifically before deciding to meet with a certain practice.
While everyone has a different opinion on what is most important here are some common questions to ask yourself when researching a veterinarian for your cat:
- Does the place have a good reputation? How long have they been in practice?
- Are the facilities clean and updated?
- Are their other patients in the office? This can be a good indicator that other cat parents trust this particular veterinarian.
- Are they timely at responding to questions or at seeing your cat at your scheduled appointment time?
- Is the staff friendly?
Follow Your Instincts
Look to a vet’s website to find answers to the issues most important to you. If you can’t find answers online, don’t hesitate to call the office and ask these questions before making an appointment. You can even ask to come in and meet the vet without your cat. Once you do, ask him or her questions and follow your instincts. Is this someone you feel like you can trust with your cat even if you’re not in the room?
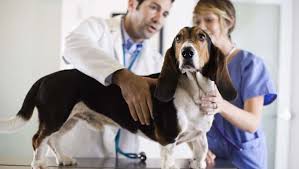
How to Find the Right Veterinarian for Your Dog
Every dog deserves a good veterinarian to help it stay healthy. As a pet owner, you also deserve a veterinarian who meets your needs a well as your dog’s needs. Your veterinarian is your other family doctor, so you want to find the right one. Here’s how to go about finding the right vet for you and your family.
Before You Begin
There are many different types of veterinarians out there. There are also a lot of different veterinary facilities. Remember that your vet will come with a staff, facility amenities, and more. Decide what matters most to you. Are you looking for a highly skilled vet in a state-of-the-art facility that offers a personal touch? Or, would you prefer a quick, inexpensive vet visit with a no-frills approach? Of course, there are options in-between. Cost is almost always a concern, as well as location, but these should not be the only things you consider. Make a list of your ideal veterinarian’s attributes in order of priority. Once you have an idea of what you need in veterinary practice, it’s time to do your research.
What You Need
In selecting a vet, you need to spend some time and energy to make the right choice. As you gather information, make sure you have some essential questions and concerns about the choices.
- A file (online or paper) to keep your notes
- List of questions you’ll want to ask the vet
Talk to People
Friends, family, and neighbors may offer great insight when you are searching for the right veterinarian. These are people you can usually trust to tell you the whole truth about their experiences, both good and bad. You may also consider asking trusted professionals/businesses in your area if they recommend and specific veterinarians. Ask why they recommend that vet so you can determine if the qualities they describe align with your personal needs and wants.
Ask for Recommendations
One of the best ways to find a great veterinarian in your area is to ask for recommendations from friends, family, and people who work with animals locally, such as your trainer, groomer or breeder, a local boarding kennel employee, or pet sitter. It’s important to find people who share your attitudes towards animals, and who have the same sort of animal, as different pets have different needs.
If you are moving to a new area, ask your current veterinarian for a recommendation, and/or check with local area veterinary medical associations for a list of active members.
Check the Websites of Local Animal Hospitals, Clinics and Practices
A slick website does not necessarily mean the clinic or veterinarian is highly rated. Conversely, it’s also possible for an excellent veterinarian to have a terrible website (or none at all). It’s useful to check online for some of the practical aspects of your search, however. Most websites should offer important details, such as hours of operation, so you’ll know if the clinic is open during times that are convenient for you.
You should also be able to see the location of the practice and if parking or public transport is available. It’s more convenient if you can find a good veterinarian who is geographically close to you, since it will be much easier if you have an emergency and need to see them quickly. Proximity isn’t the most important factor, however. You might decide that it’s better to travel farther for someone who has a better reputation or a particular specialty.
Preventing Problems During the Vet Selection
It’s probably best to leave your dog out of the equation until you find a vet you like. It will only confuse and stress the dog out if you are bringing your dog on multiple visits to meet a vet. And, if the vet you have selected is not ideal or not working out, don’t worry too much. Refer back to your research, pick a new vet, and move on. Do pick someone as soon as possible; you don’t want to be a dog owner without a vet on standby for any health problems.
Pain Management For Shoulder Pain
What Are the Treatments for Chronic Pain?
The treatments for chronic pain are as diverse as the causes. From over-the-counter and prescription drugs to mind/body techniques to acupuncture, there are a lot of approaches. But when it comes to treating chronic pain, no single technique is guaranteed to produce complete pain relief. Relief may be found by using a combination of treatment options.
Types of Pain
Acute pain can last a moment; rarely does it become chronic pain. Chronic pain persists for long periods. It is resistant to most medical treatments and cause severe problems.
Pain Classifications
Even though the experience of pain varies from one person to the next, it is possible to categorize the different types of pain.
Chronic Pain
Learn about how chronic pain occurs, and why chronic pain sometimes lingers.
Nerve Pain
When nerve fibers get damaged, the result can be chronic pain. Read about the very common causes of neuropathic pain, like diabetes.
Psychogenic Pain
Depression, anxiety, and other emotional problems can cause pain — or make existing pain worse.
Musculoskeletal Pain
Musculoskeletal pain is pain that affects the muscles, ligaments and tendons, and bones. Learn about the causes, symptoms, and treatments.
Chronic Muscle Pain
Use your muscles incorrectly, too much, too little — and you’ve got muscle pain. Learn the subtle differences of muscle injuries and pain.
Abdominal Pain
Learn common causes of abdominal pain and when to contact your doctor.
Joint Pain
See the causes of joint pain and how to treat it with both home remedies and prescribed medication.
Central Pain Syndrome
A stroke, multiple sclerosis, or spinal cord injuries can result in chronic pain and burning syndromes from damage to brain regions. Read this brief overview.
Chronic pain: Medication decisions
Chronic pain: Medication decisions
Chronic pain can limit your quality of life and lead to additional, serious health problems. Finding effective treatment is important — as is balancing pain relief with your safety.
Chronic pain is a serious health condition. Like any long-term health problem, the condition often leads to complications beyond your physical symptoms, such as new or worsened depression, anxiety and difficulty sleeping. Chronic pain can make it more difficult to keep up at work, manage tasks at home and attend social gatherings, leading to problems in your relationships and financial instability. Some research suggests that the more severe your pain, the more serious these problems.
Working in partnership with your doctor, however, you can identify treatments that allow you to live an enjoyable, fulfilling life. The approach you choose should include more than just medication, but painkillers are likely to play a role. Learn about the risks and benefits of common pain medications so that you can make safe choices as you seek your solution.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
NSAIDs are most effective for mild to moderate pain that’s accompanied by swelling and inflammation. These drugs are commonly used for arthritis and pain resulting from muscle sprains, strains, back and neck injuries, or menstrual cramps.
- Generic (brand) names. Ibuprofen (Advil, Motrin IB, others); naproxen sodium (Aleve); others
- How they work. NSAIDs work by inhibiting certain enzymes in your body, called cyclooxygenase, that are released during tissue damage. By blocking the different types of cyclooxygenase (COX) — including COX-1 and COX-2 — NSAIDs can help reduce pain and inflammation that result from an injury.
- Benefits and risks. When taken as directed, NSAIDs are generally safe. But if you take more than the recommended dosage — and sometimes even just the recommended dosage — NSAIDs may cause nausea, stomach pain, stomach bleeding or ulcers. Large doses of NSAIDs can also lead to kidney problems, fluid retention and high blood pressure. Risk of these conditions increases with age and in the presence of other health problems, including diabetes, a history of stomach ulcers or reflux, and kidney disease.
- Bottom line. If you regularly take NSAIDs, talk to your doctor so that he or she can monitor you for possible side effects. Bear in mind that NSAIDs also have a ceiling effect — a limit as to how much pain they can control. This means that beyond a certain dosage, they don’t provide additional benefit. Exceeding the recommended dose may not relieve your pain and may increase your risk of serious side effects.
Acetaminophen
Acetaminophen is usually recommended as a first line treatment for mild to moderate pain, such as from a skin injury, headache or musculoskeletal condition. Acetaminophen is often prescribed to help manage osteoarthritis and back pain. It may also be combined with opioids to reduce the amount of opioid needed.
- Brand names. Acetaminophen (Tylenol, others)
- How it works. Doctors don’t know exactly how acetaminophen works. Some scientists believe there may be a third type of cyclooxygenase, COX-3, that acetaminophen blocks. Acetaminophen doesn’t affect the other two cyclooxygenase enzymes, and it doesn’t target inflammation — only pain. It may be less effective than NSAIDs.
- Benefits and risks. Acetaminophen is generally considered safer than other nonopioid pain relievers because it doesn’t cause side effects such as stomach pain and bleeding. However, taking more than the recommended dose — or taking acetaminophen with alcohol — increases your risk of kidney damage and liver failure over time.
- Bottom line. Acetaminophen is generally a safe option to try first for many types of pain, including chronic pain. Ask your doctor for guidance about other medications to avoid while taking acetaminophen. Acetaminophen is not as effective as NSAIDs for the treatment of knee and hip pain related to osteoarthritis.
COX-2 inhibitors
These medications were developed with the aim of reducing common side effects associated with traditional NSAIDs. COX-2 inhibitors are commonly used for arthritis and pain resulting from muscle sprains, strains, back and neck injuries, or menstrual cramps. They are as effective as NSAIDs and may be the right choice if you need long-term pain control without increased risk of stomach damage.
- Brand names. Celecoxib (Celebrex)
- How they work. COX-2 inhibitors, another type of NSAID, work slightly differently from traditional NSAIDs. A COX-2 inhibitor blocks only the COX-2 enzyme — the one that’s more likely to cause pain and inflammation.
- Benefits and risks. COX-1 enzymes help protect the lining of your stomach. NSAIDs, which block COX-1, can cause side effects such as stomach pain and bleeding. COX-2 inhibitors, on the other hand, help keep the stomach protected by acting only on COX-2 enzymes, allowing COX-1 to function normally.
- Although the risk of stomach bleeding is generally lower if you take a COX-2 inhibitor instead of an NSAID, bleeding can still occur, especially at higher doses. These medications may cause side effects, such as headache and dizziness, and can lead to kidney problems, fluid retention and high blood pressure.
- Bottom line. Older adults may be at higher risk of common COX-2 side effects compared with younger adults. If these medications help you manage chronic pain, aim to take the lowest effective dose for the shortest time possible, and follow up closely with your doctor.

What Are Corticosteroids?
Prescription corticosteroids provide relief for inflamed areas of the body by easing swelling, redness, itching and allergic reactions. Corticosteroids can be used to treat allergies, asthma and arthritis. When used to control pain, they are generally given in the form of pills or injections that target a certain joint. Examples include: prednisone, prednisolone, and methylprednisolone.
Prescription corticosteroids are strong medicines and may have serious side effects, including:
- Weight gain and salt retention
- Peptic ulcer disease
- Mood changes
- Trouble sleeping
- Weakened immune system
- Thinning of the bones and skin
- High sugar levels
To minimize these potential side effects, corticosteroids are prescribed in the lowest dose possible for as short of a length of time as needed to relieve the pain.
The impact of chronic pain
Chronic pain can have an enormous impact on people. It may interfere with a person’s sleep patterns, their sexual activity, their ability to work and conduct daily activities, and it can cause emotional distress and lead to serious mental health problems, including depression.
The goals of pain treatment are to enhance functioning and reduce suffering and distress, while minimising the risk of adverse effects. While it is rare to eliminate chronic pain completely, it should be possible to control pain to a tolerable level and allow people to function at an acceptable level.
While acute pain can usually be attributed to an identifiable disease or damage process, finding an identifiable process for chronic pain can be very difficult. Sometimes the cause of the pain cannot be determined. This does not make the pain any less real to the patient.
Dermatologist Skin Care Products
HOW TO BECOME A DERMATOLOGIST
Required Education
Prospective dermatologists must first obtain a bachelor’s degree, taking courses in English, math, inorganic and organic chemistry, physics, and biology. Then they must complete medical school, where they’ll spend the first two years studying human anatomy and physiology, microbiology, pathology, and medical ethics, among other subjects.
During the last two years, they’ll work with hospital patients under the supervision of staff doctors. Graduation from medical school is followed by a one-year year internship, three years of on-the-job training as a medical resident, a state-licensing exam, as well as a certification by the American Board of Dermatology (ABD) for those who qualify.
Skills Required
Dermatologists must be emotionally stable, motivated to serve others, able to work long hours, and willing to engage in lifelong learning. Compassion for patients and good communication, organization, and problem-solving skills are key. Dermatologists should also be detail oriented, manually dexterous, and patient when dealing with individuals or young children who are anxious about treatments.
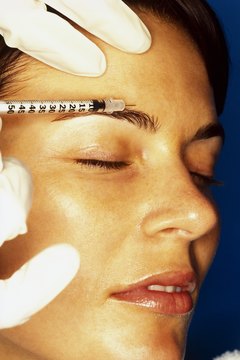
PLAN ACCORDINGLY: IT TAKES OVER A DECADE TO BECOME A DERM.
Like any medical professional, becoming a dermatologist requires *years* of schooling. Aside from earning your bachelor’s degree, you must attend an additional four years of medical school. After passing several major exams, you then apply to a residency, which takes another four years to complete. Some people choose to focus on sub-specialties within the field, such as cosmetic or surgical dermatology, and in that case, it takes another year or two to complete a fellowship. All in all, expect a bare minimum of 12 years of schooling before becoming a certified dermatologist.
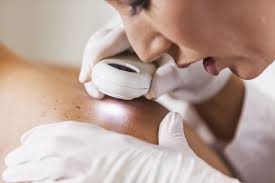
REWARDS OF BEING A DERMATOLOGIST
Dermatologists treat skin, hair and nail disorders, and some beautify a person’s appearance. Enter the field of dermatology and you’ll reap the rewards, from a bank account that can see a huge deposit of money each payday to a work week that doesn’t see you chained to the desk for hours on end. But those benefits aren’t easy to come by — dermatology is a highly competitive field to get into.
High Salary
If you enjoy the sight of Benjamin Franklin’s face on money, you’ll love being a dermatologist. Physicians in general earn boatloads of money, but dermatologists really rake in the greenbacks, to the tune of an average of $283,000 in 2011, according to Medscape’s 2012 Physician Compensation Report compiled from survey results. That number hides an important statistic: women dermatologists earned significantly less than men. Women earned an average annual salary of $252,000, while men pulled in 24 percent more at $313,000. The average annual salary for all physicians in 2012 was $184,820, according to the U.S. Bureau of Labor Statistics.
Reasonable Work Week
Putting in long hours at work often translates to more stress. That’s not as much of a concern for a dermatologist. According to Medscape’s 2012 Physician Compensation Report, 52 percent of dermatologists reported spending between 30 and 40 hours per week in direct patient care. Only 30 percent of all physicians surveyed said they worked similar hours — most worked more. Working fewer hours each week than you would in another specialty gives you plenty of free time to spend with your family, your dog, yourself or with hundreds of other people at the mall, spending a chunk of that massive paycheck.
Perform Surgeries and Variety of Patients
Many physicians don’t have the option of treating their patients’ conditions non-surgically and surgically. It’s usually one or the other. Think of your family doctor: if you need your wrist operated on, a kidney stone taken out or anything that requires a surgical approach, he’s not going to be the one who does it. Dermatologists are trained in surgical and non-surgical procedures, injecting some variety into their career and making their work week a little less routine. Speaking of variety, become a dermatologist and you’ll treat patients from all walks of life, from little rascals who have a bad case of acne to adults who want their wrinkly skin to be a thing of the past.
High Demand
In most communities, dermatologists are some seriously sought-after docs. Skin conditions are prevalent in most age groups. Teens often go through bouts of acne, older men and women aren’t awfully excited about losing their hair, people want treatment for their varicose veins, and skin cancer, thanks largely to tanning beds, is rearing its ugly head more and more. Beyond medical conditions that need to be treated, cosmetic fixer-uppers are also often requested, especially when the economy is trucking along and people have more disposable income.

PROS AND CONS OF CHOOSING DERMATOLOGY
This article is for you if you’re in the throes of med school. You’re probably in survival mode, subsisting on caffeine and adrenaline – but you are probably also giving some thought, when you can, to what comes next. Where do you want your professional career to take you? Perhaps – dermatology?
Of course, as a specialty, the years of schooling – and associated cost – are something to consider thoroughly before taking on dermatology as your chosen path. Many agree that dermatology is a specialty that requires some of the highest performances, academically, to enter.
But the eventual salaries can make up for that, with averages among the highest in any specialty, and growing. It’s possible that future compensation could fall, as managed care continues to evolve and affect the practice of medicine. But, for now, dermatologists ranked among the highest on job satisfaction overall.
Job growth is projected to be very promising, as it’s a small community. While dermatology saw a rise in burnout rates over the last few years, the rate is comparatively very low, according to a recent study. There can be lower feelings of stress, possibly because the profession is so well compensated and because most cases are not time-critical (unlike, for instance, those of an emergency medicine specialist).
However, some say that dermatology can have little respect in the overall physician community. This may be because some see dermatology as one of the “lighter” specialties, with a focus on wrinkles and other lifestyle, rather than foundational, health concerns.
DERMATOLOGISTS – PREPARATION
To work as a dermatologist, you typically need to:
- have a high school diploma or equivalent;
- complete a bachelor’s degree;
- graduate from medical school;
- complete an internship;
- pass a state licensing exam;
- complete a residency program in dermatology; and
- pass additional exams to become board certified.
EDUCATION AFTER HIGH SCHOOL
To become a dermatologist, you must complete medical school. Medical schools grant a Doctor of Medicine (MD) degree. You spend the first two years of medical school in classrooms and labs. You study anatomy, biochemistry, and medicines. You also learn how to take a medical history, examine patients, and make a diagnosis. During the next two years, you work in hospitals and clinics under the supervision of physicians.
You need a bachelor’s degree to get into medical school. While you do not need to be a pre-medicine or science major, these programs are good preparation. If you earn a liberal arts degree, be sure to take courses in physics, biology, and chemistry.
WORK EXPERIENCE
It takes 12 to 14 years to become a dermatologist. It’s a good idea to decide early if dermatology is the right specialty for you. Volunteer to work in a dermatology office while still in college. Take a paid position as a medical assistant in a dermatology practice. Talk to people in this field and find out what they like about it and what skills and qualities are necessary. A helpful dermatologist may allow you to shadow them for a day or a couple of weeks. This will help you determine if this specialty is right for you.
ON-THE-JOB TRAINING
While in medical school, you spend two years working as an intern in a hospital or clinic. As an intern, you rotate through internal medicine, family medicine, obstetrics, oncology, and other hospital departments.
After medical school, you complete a residency program in dermatology. Residency lasts up to five years. After your residency, you take additional exams to become board certified.
Pediatric Nursing Isn’t Just Kids Stuff
How to Choose a Pediatrician
Pediatricians have special training in the health and illnesses of children from birth through adolescence and into the young adult years, and most are certified by the American Board of Pediatrics after passing a comprehensive examination covering all areas of health related to infants, children, and young adults
How to Find the Names of Qualified Pediatricians
The American Academy of Pediatrics and HealthyChildren.org can supply you with names of board-certified pediatricians in your community through our Find a Pediatrician tool.
*Note: Only Fellows of the American Academy of Pediatrics or “FAAPs” are listed in our Find a Pediatrician tool. Only board-certified pediatricians can add the designation “FAAP” after their names, which means they have reached the highest status of membership in this professional organization.
Most local/county medical societies provide referral services to pediatricians in their area who are taking new patients.
If you are located near a major medical center, community hospital, or teaching hospital, contact its department of pediatrics for the names of doctors in your area
Interviewing Pediatricians
With a list of doctors in hand, call the office of each. Explain that you are looking for a pediatrician for your child, and inquire about the doctor’s background and training, as well as general office procedures. If you are impressed with what you hear, arrange for an interview during which you can meet the doctor and ask some additional questions. It may be more convenient to do this interview by telephone
Here are some key questions to ask and things to consider during this first meeting:
What medical school did the pediatrician attend, and where did he or she undergo postgraduate and residency training? (Medical directories in many public libraries and online—such as the American Board of Medical Specialists Directory—can also help answer these questions.)
What are the doctor’s present hospital appointments? If it becomes necessary for your child to be hospitalized, where would he or she be admitted?
Is the pediatrician’s office conveniently located? Is it easily accessible by car or public transportation?
Are the office hours convenient for your own schedule? If you are a working parent, you may desire evening or weekend hours.
What is the doctor’s policy on taking and returning phone calls? Is there a nurse in the office who can answer routine questions?
Is the doctor in a group practice with other physicians? Does another physician cover for the doctor at times? Who handles phone calls when the office is closed or during vacations?
Do you sense a genuine interest by the doctor in the problems of your child, including particular health disorders he or she may have?
Do both the physician and the office staff appear amicable and courteous? Do they demonstrate compassion and patience? Or do you feel rushed in the office, as though the doctor is eager to move on to the next patient?
How are visits for acute illnesses handled? Can you make an appointment on short notice if your child needs to see the pediatrician because of a sore throat, cold, or a potential ear infection, for example?
Does the doctor communicate clearly to explain illnesses and treatments, and does the doctor make an effort to ensure that all your questions are answered?
In what managed-care programs does the doctor participate? What is the office policy regarding the processing of insurance forms?
What will be the fees you will be responsible for when seeing the doctor for sick visits, routine examinations, etc.? See Understanding Cost Sharing: Deductibles, Copayments & Coinsurance.
If your child ever develops a complex illness that requires he care of one or more specialists, will your pediatrician coordinate care among all the doctors providing treatment? See Your Child’s Medical Home: What You Need to Know.

How to Select a Pediatrician
Choosing a pediatrician for your baby is no easy task. After all, this doctor will help your little one through childhood vaccinations, nasty colds, and everything in between. But when should you start looking for a pediatrician, and what criteria should you focus on? Here are our top tips for choosing the best pediatrician near you.
When Should I Look For a Pediatrician?
Start looking for pediatricians while you’re still pregnant—preferably between 28 and 34 weeks along. “It’s important to have a pediatrician you’ve already met and respect, because you have enough going on after the baby is born,” says Evaline Alessandrini, M.D., a pediatrician at the Children’s Hospital of Philadelphia.
There’s also another benefit of finding a pediatrician early: Dr. Alessandrini’s recent study, which she co-authored, found that babies who see the same doctor for their first 6 months are up to twice as likely to receive important health tests before they turn 2. Sticking with the same doctor also prevents wasted time on things like “going over whether immunizations are up to date,” she says. “If you have a continuing relationship with a doctor, you have the time and comfort to go deeper.”
How to Research a Pediatrician
Searching for a pediatrician may seem daunting, but remember that you’re not trying to find “the best doctor in the world.” You’re simply looking for the most effective doctor for you, your partner, and your future child. Here are some tips.
Get references. Everyone has different criteria for picking a pediatrician, so you should collect at least three names from friends and coworkers. (If you’re short on preferred doctors, try the American Academy of Pediatrics’ referral site at aap.org/referral.) Also look into the hospitals that your candidates are affiliated with; you’ll want one that’s both convenient and reputable.
How to Choose the Best Pediatrician for Your Child
Parents seem to go to a lot of different extremes when choosing a pediatrician. Some do almost nothing and simply choose the pediatrician on call in the hospital when their baby is born or pick a doctor randomly from a list in the phone book or their insurance directory.
The Importance of Choosing a Pediatrician
Choosing the right pediatrician is more important than most parents think. While you can simply change doctors if you don’t like the first pediatrician you see, if your newborn or older child is truly sick, the first doctor you see could be making life-changing decisions about your child. Or they could miss a potentially life-threatening problem.
Pediatrician Recommendations
A common way for parents to choose a pediatrician is to get a recommendation from their friends or family members. This is probably one of the best ways, but when someone tells you that they love going to their pediatrician, be sure to ask why before you blindly follow them to the same office.
Choosing a Pediatrician
Although we like to think that things like cost and convenience should be secondary when making such an important decision, they can be very important when choosing a pediatrician. If the pediatrician you would like to see is not on your insurance plan or is an hour away, it may not be very practical to go to her office.
Interviewing Pediatricians
Although you can typically narrow down your choice of pediatricians by figuring out who is on your insurance plan and in your area, who is accepting new patients and getting some recommendations from friends and family, the best way to find a good pediatrician is to actually set up an appointment and meet with a few.
How to Choose a Pediatrician
When looking for a pediatrician to care for your baby, you’ll want to give yourself plenty of time to find someone both you and your partner feel comfortable with. So it’s a good idea to begin choosing a pediatrician at the beginning of your third trimester. Ask your OB and trusted family and friends for recommendations.
These questions can help you choose the right pediatrician for you.
Does this doctor have a good reputation?
What is this doctor’s training and experience?
Does the pediatrician respect my philosophy on breastfeeding and immunizations?
Does the doctor listen to me and explain things clearly?
Will my child see the same doctor every time?
Who covers for the pediatrician when he or she is not available?
Is my spouse or partner comfortable with this doctor?
Is the office staff pleasant and helpful?
Is the office location convenient?
How long does it take to get an appointment?
How long will my child and I spend in the waiting room?
Does the pediatrician offer evening and weekend hours? Who sees my child during these hours?
How are emergencies and after-hour calls handled?
What hospital is the pediatrician affiliated with?
Does my insurance cover this doctor’s services?

How to Choose a Pediatrician: What to Look For
Choosing the right doctor for your child is one of the most important decisions you’ll make for you and your baby. Sure, you’ll want to consider convenience and office hours: Is it close to home, are they open late or on weekends? What about expertise — where did they do their training, are they board-certified? Do they come recommended by friends and family? What’s their philosophy on things important to you?
Convenience
It can help to look for a practice that fits into your life and can support you, too, by being there when you need them. You’ll want both convenience and quality care, from a doctor you can trust to be on your side through your child’s development and growth. A good pediatrician will be available to your entire family to offer advice from infancy through adolescence
Values
A good pediatrician knows how to listen to you and your child. They understand the unique needs of parents and young families and can dispel myths, alleviate fears, and provide information you need — at the right time. You want someone who you can speak to honestly and collaborate with on the care of your child.
Expertise
Consider the level of training of the provider who will care for your child. Are they board-certified in pediatrics? Do they offer specialized training in breastfeeding, child development, or other things that will meet your family’s needs? And does the practice have direct access to pediatric specialists, if and when they need them, for reference or advice?
Make an informed choice
Becoming a parent or growing your family is a time of huge transition. It can, at times, feel like a rollercoaster ride. But it’s all part of the process; the joys and challenges of being a great parent. And when your child is here, having the right pediatrician by your side can make all the difference in the world.